In March 2014, a team of researchers led by Sue O’Shea, Ph.D., and Melvin McInnis, M.D., published a report of the first stem cell lines (iPSC) generated from patients with bipolar disorder. This is a powerful model to study cell function, and will stimulate the discovery of new molecules to develop and test new medications.
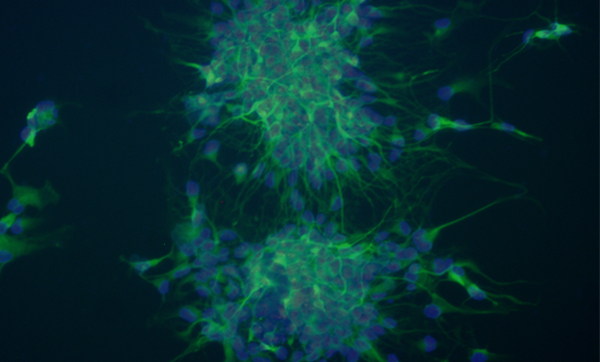
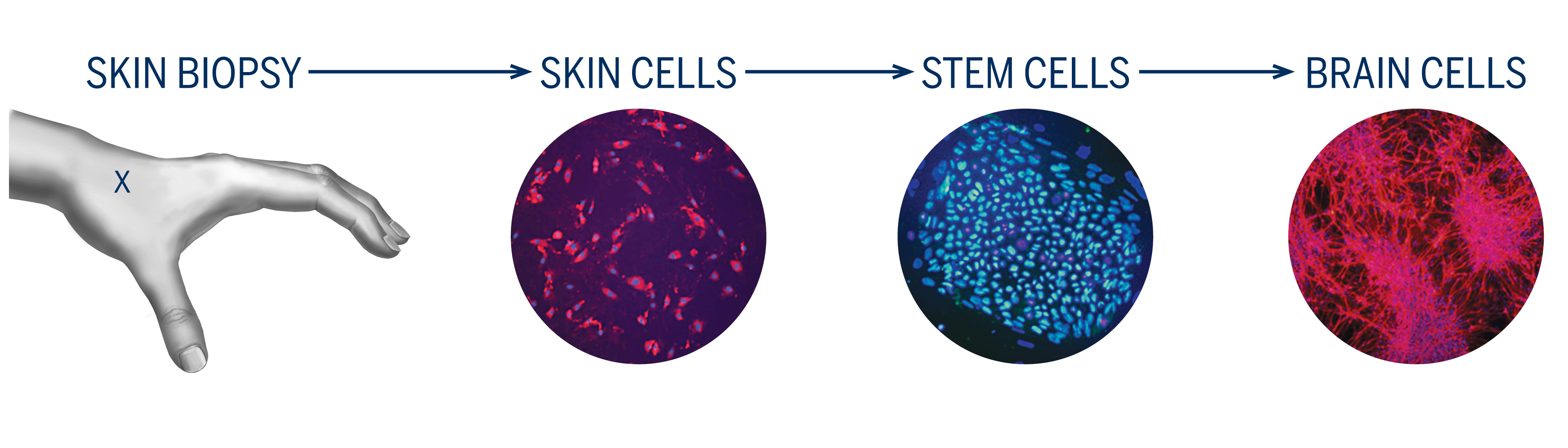
Dr. O’Shea’s lab, where she directs eight researchers, is working to derive induced pluripotent stem cells (iPSC) from skin biopsies from patients diagnosed with bipolar disorder and control individuals. This exciting project involves sampling skin tissue from adults with and without the illness, and transforming those cells into stem cells and ultimately into nerve cells that look and behave like brain cells.
This allows us to understand — in a laboratory — how individuals might react to different treatments and it is truly the heart of “personalized medicine.” We believe this novel research will lead to treatments based on each individual’s unique cellular profile. The Prechter Bipolar Research Program is a strong leader of biomedical research in bipolar disorder.
Bipolar Disorder in a Culture Dish
Mood disorders are devastating brain illnesses that are major causes of disability and mortality worldwide. Better treatments are needed, but without living brain cells to study, progress has been limited. This project develops bipolar neurons in culture to overcome this hurdle. We are turning skin cells from bipolar patients into stem cells and then turn those stem cells into neurons, or brain nerve cells, as illustrated in the diagram. Responses of bipolar neurons to new treatments are being compared with responses from neurons derived from controls.
The goals of the laboratory are to understand the differences between nerve cells from bipolar and control individuals so that they can be more effectively treated by medicines or electroshock procedures. Personalized treatments — those that work for each individual — are now achievable goals.
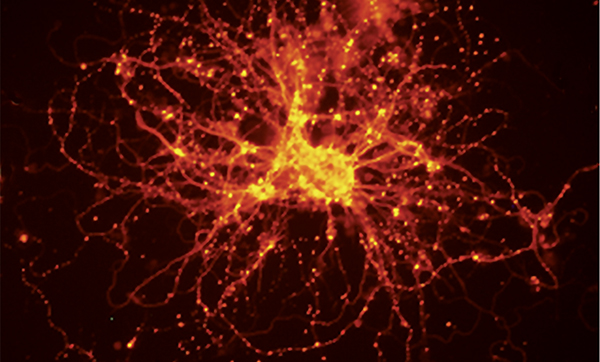
Nerve cells from a bipolar patient. The branches (red) are the cables that run through the nervous system carrying nerve signals. The bright yellow spots are synapses and show where cells communicate with each other. The nerve signals in bipolar nerve cells are stronger and longer compared to non-bipolar nerve cells.