Advancing Musculoskeletal Health
Orthopaedists interact with patients throughout their lives, which allows us to impact a patient’s quality of life, their whole life long.
Our diverse clinical faculty have specialized training in sports medicine and shoulder surgery, pediatric orthopaedics, joint reconstructive surgery, orthopaedic trauma and fractures, hand and upper extremity surgery, foot and ankle surgery, spine surgery and orthopaedic oncology. The Department of Orthopaedic Surgery comprises nearly 30 faculty with interests in a broad range of clinical areas, research and education.
To enhance patient care, the department is organized by clinical services.
Our surgeons have training in a variety of specialty areas, and our unique approach, specialty clinics and top-ranked programs are the most comprehensive in Michigan and the country.
We specialize in the care of patients with both common and complex disorders of the foot and ankle. Our staff provides superior, comprehensive foot and ankle treatment for patients in a clinical atmosphere that is caring and responsive to current and long-term patient needs. We specialize in traditional, innovative and safe surgical services of the forefoot, midfoot, hindfoot and ankle.
The Hand Clinic fully diagnoses and treats the complete range of hand problems. From fractures and congenital anomalies to deformities from arthritis and trauma, the U-M Hand Clinic offers specialized treatment. We are able to treat the smallest vessels in the hand and upper body.
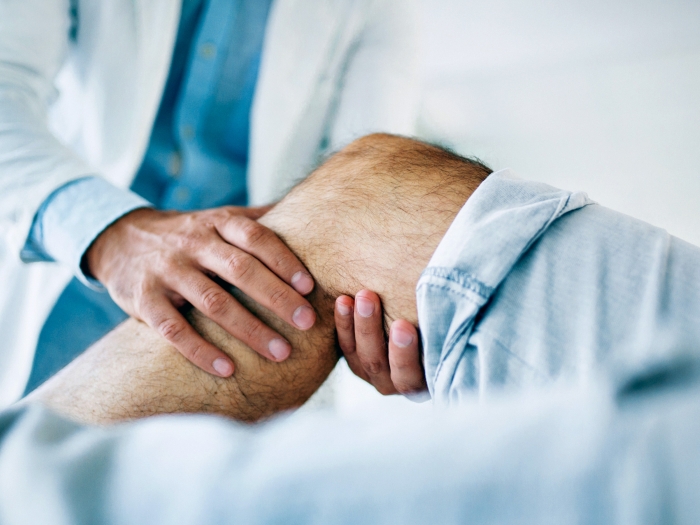
We lead the field in the prognosis and treatment of hip and knee related conditions. We offer primary and revision total hip and knee replacements and point preservation surgery, including hip dysplasia osteotomies, femoro-acetabular impingement treatment, both open and arthroscopic.
The Musculoskeletal Oncology Service specializes in treating soft tissue and bone tumors of the limbs, pelvis, and shoulders, benign and malignant tumors, metastatic disease of bone, primary bone malignancy, sarcoma, and pathologic fractures due to malignancy in children and adults. Bone cancer treatment often involves a multidisciplinary approach involving several specialists such as orthopaedic oncology, medical oncology, radiation oncology, radiology and pathology.
The Pediatric Orthopaedic Surgery Service specializes in all aspects of musculoskeletal care for infants, children and adolescents. This expertise includes diagnosis as well as surgical and nonsurgical treatment for a wide range of problems such as skeletal deformities, musculoskeletal diseases and traumatic injuries.
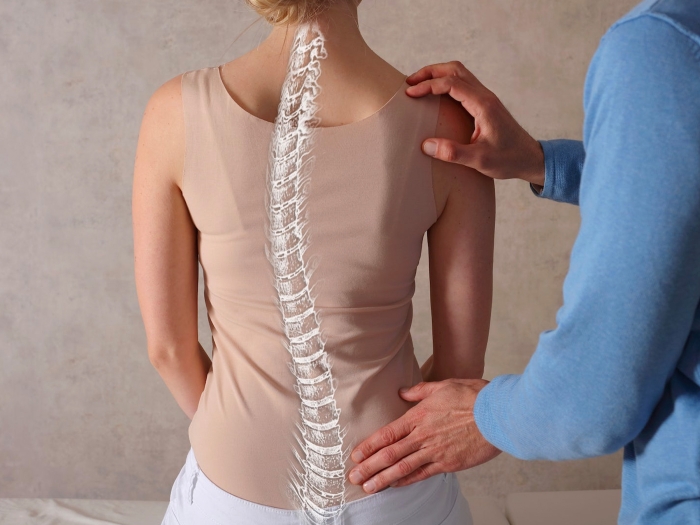
The University of Michigan Spine Surgery Program provides comprehensive, cutting edge treatment options to patients with neck and back disorders. Our surgeons specialize in the diagnosis and treatment of patients with scoliosis or spinal deformities, spinal cord or nerve compression, tumors of the spine, and neck or back pain. Our experts offer a broad spectrum of surgical options including minimally invasive spine surgery, kyphoplasty, complex spinal revision and reconstructive surgery.
We provide complete sports medicine services for musculoskeletal orthopaedic-related injuries and conditions, including injuries to the knee, elbow, shoulder and more. We also promote research and educational opportunities in sports medicine for our staff and students using a team approach that incorporates physicians, physician assistants, physical therapists and certified athletic trainers.
The Orthopaedic Trauma and Fracture service provides primary and referral care for skeletal trauma and fractures as well as problems related to improperly healed fractures (delayed bone healing, missing or short bones, “nonunions”, crookedly healed bones). Our team has expertise in guiding you or a loved one through fractures from the shoulder to the forearm, the hip to the ankle / hindfoot for adults and fractures of the pelvis and acetabulum throughout the entire lifespan. We share the most up-to-date knowledge and employ the latest evidence-based techniques when surgery is needed.